Thumb/Wrist Pain? It could be De Quervain’s Tenosynovitis.
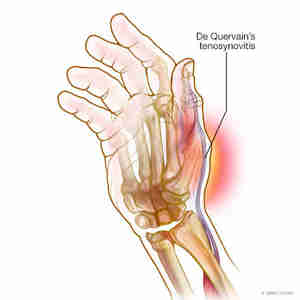
De Quervain’s Tenosynovitis is a painful condition which affects the thumb muscles including Abductor Pollicis Longus and Extensor Pollicis Brevis. A smaller muscle, called Abductor Pollicis Brevis can also be impacted.
Why does it happen and who is at risk?
Females are 4x more likely then men to develop Abductor Pollicis Brevis Pain. It is particularly prevalent in women who are in the post-natal phase. It is caused by a rapid increase in load on the thumb muscles and tendons. This over-load is usually caused from repetitive lifting of your new bub out of the cot and feeding positions with the wrist in a flexed position. It can also commonly occur in golfers, waiters and carpenters due to repetitive action of the wrist and thumb.
Tendons typically take an extended period to adapt to new loads and if we introduce new loads too quickly (same as when an Achilles tendon gets sore when you first start running training), they get a bit grumpy!
Signs and Symptoms of Abductor Pollicis Pain (De Quervain’s)
Symptoms will include swelling and local tenderness over the tendons on the thumb side of the wrist. You may experience a sudden sharp feeling when lifting your child or even lifting pots/pans etc. It can sometimes throb/ache for a while after aggravating it.
It won’t present with any nerve symptoms like pins and needles or numbness so if you do experience these symptoms, it is more likely there is a nerve impingement issue higher up in the elbow (posterior interosseous nerve) or in the neck.
Diagnosis
It is diagnosed by conducting a simple test called the Finkelstein test. The tests involve bending your thumb across the palm of your hand and then bending your fingers over the thumb. The wrist is then bent toward your little finger, called ulnar deviation. If this reproduces the same pain you experience and is not painful on your other, unaffected hand, it is likely De Quervains syndrome.
A physiotherapist will also conduct some tests on the joints around the thumb and wrist and some nerve tests to exclude them as a source of pain.
De Quervain’s Tenosynovitis Treatment
- Splinting. Successful De Quervain’s treatment techniques include splinting/bracing of the wrist to off-load the thumb tendons, and then progressive weaning from the brace to reintroduce load in a monitored way. Splinting is normally started at night only, unless the symptoms are severe, in which case we recommend wearing it all day for at least 2 weeks initially. This simply gives the tendons a chance to rest and recover.
- Gradual strengthening of the tendon is highly important as increasing the tendons tolerance to load is the fundamental component of rehab. As with any tendon strength program, load needs to be slowly introduced as a sudden increase in strength exercises can easily overload and aggravate the tendon. If bracing is left on for too long the tendon will become weaker and hence when you remove the brace the pain will come back.
- Despite common belief, a corticosteroid injection is not the first-line treatment. An injection should only be considered if bracing and physiotherapy has failed over a 6-week period OR if the symptoms are severe enough to warrant an early.
If you start treatment early, your symptoms should improve over the next 4-6 weeks. If your symptoms start during or after pregnancy your symptoms are likely to resolve once breast feeding has stopped.
TOP TIPS:
-
ICE for pain relief
-
BRACE to off-load the tendon
-
STRENGTH to increase the tendons tolerance to load (likely the reason the thumb was sore in the first place).
-
CORTISONE injection only after 6 weeks if the above fails.
If you have any questions or if you think you may have De Quervain’s then please do not hesitate to get in touch with us here.