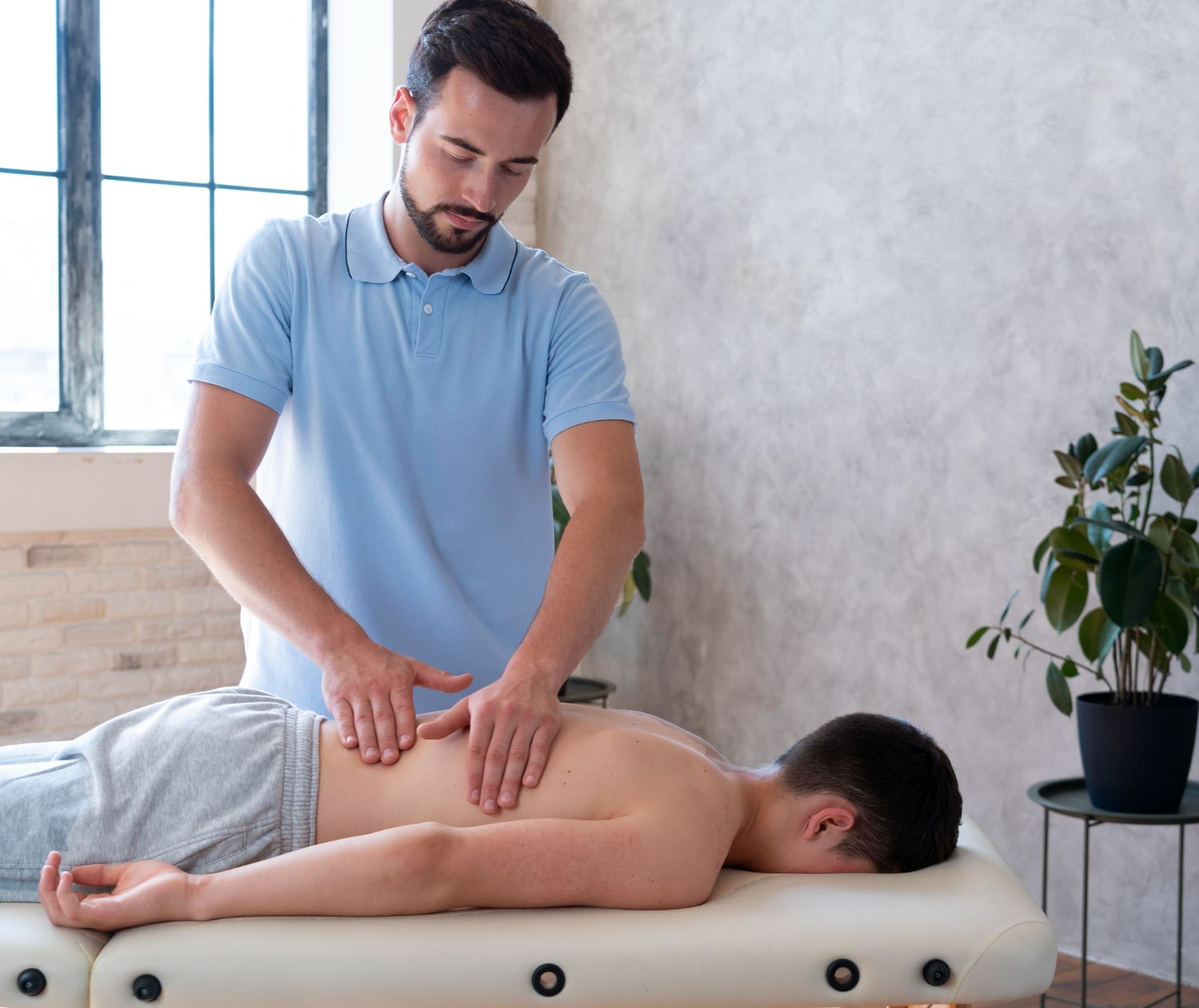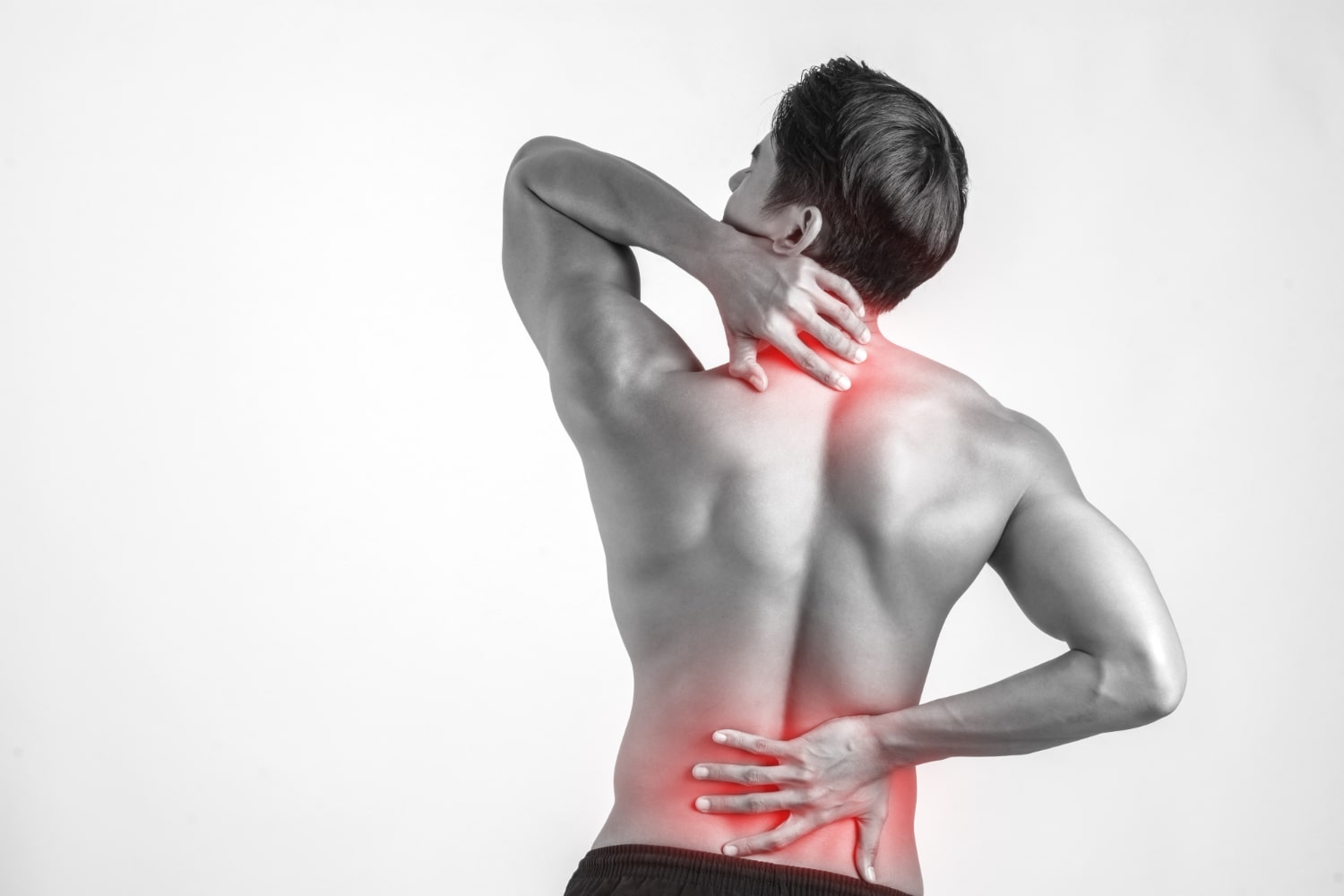
Clinical Physiotherapy for Lower Back & Neck Pain
“Treatment of both acute and chronic lower back pain should include a combination of manual therapy (manipulations/mobilisations) and an appropriate, progressive exercise program.”
George et al 2021 “Clinical Practice Guideline – Interventions for the Management of Acute and Chronic Low Back Pain: Revision 2021″.
Journal of Orthopaedic and Sports Rehabilitation
Our team are trained in the most up to date, evidence-based treatments for the following spinal conditions:
Neck Pain
Acute neck pain or “Wry Neck”
- How does it happen?
Characterised by an acute onset of neck pain with protective deformity and limitation of movement. Commonly occurs after a sudden, quick movement or on waking. - Risk factors
– High-stress levels
– Sudden movements; sneezing or turning head quickly
– Frequently seen in adolescents and more common in females than males.
– Sleeping on your stomach - Common symptoms
– Pain
– Loss of range of motion
– Stiffness - Common treatments and recovery expectations
Most patients recover within 4-7 days and sometimes faster if treatment is started on day Common treatments include massage, joint mobilisation, gentle stretching and advice/education.
Stiff Neck
- How does it happen?
Defined as a degenerative disorder, complicated by inflammatory reactions. Commonly referred to as Cervical Spondylosis. - Risk factors
– Previous injury
– Obesity
– Age > 55 - Common symptoms
– Pain
– Stiffness
– Crepitus
– Limited range of motion
– Joint instability - Common treatments and recovery expectations
Treatment includes conservative management of exercise therapy, mobilisation and improving overall aerobic fitness.
Chronic Neck Pain
- How does it happen?
There are a large number of reasons why someone may develop chronic neck pain. The most common reasons are non-physical in nature. For example, we commonly see people who were advised initially to not move/protect their neck and this has manifested in further complications such as stiffness, avoidance of movement due to fear and heightened pain responses to stimuli that ordinarily would not be painful. - Risk Factors
– Previous injury
– Stress
– Anxiety
– Depression
– Poor advice and/or lack of knowledge on their condition
– Muscle weakness
– Withdrawal from activity/exercise - Common symptoms
– Pain
– Stiffness
– Weakness
– Neurological symptoms - Types
– Chronic neck pain without radiculopathy (neck pain without shoulder or arm pain).
– Chronic neck pain with radiculopathy resulting from a disc bulge or other structure causing stenosis (associated with arm pain, pins and needles and numbness). - Common treatments and recovery expectations
A combination of strength and mobility exercises, postural and ergonomic strategies, manual therapy and psychological considerations are found to be the most effective in treating neck pain.
Whiplash
- How does it happen?
Acute acceleration/deceleration injury, commonly caused by a motor vehicle collision. - Risk factors
– High initial pain levels
– Neurological symptoms (pins and needles, pain referred down the arm etc). - Common symptoms
– Pain
– Stiffness
– Headaches
– Muscle spasms - Common treatments and recovery expectations
Usually, recovery time can range from a few days up to 3 months, depending on the severity of the condition. Management will be similar to Acute Wry Neck, but there is a small proportion of those who may not respond well to any treatments (medical, physical or psychological) and who generally have a poor prognosis.
Thoracic and Rib Pain
- Kyphosis
- Scheurmanns Disease
- Displaced Rib
- Costochondritis
- Costovertebral joint pain
- Costchondral joint pain
Back Pain
- Acute lower back pain (less than 6 weeks) that can be attributed to low grade muscle or ligament sprains producing pain and stiffness.
- Chronic lower back pain without radiculopathy (back pain without leg pain) which can arise from poor postural habits, aberrant movement patterns, maladaptive movement patterns, weakness of the hip extensors and stabilisers and can also be associated with a lack of, or avoidance of exercise.
- Chronic lower back pain WITH radiculopathy resulting from a disc bulge or other structure causing stenosis (associated with leg pain, sciatica, pins and needles and numbness).
Nerve Pain and Sciatica
Nerve pain can be distinguished into 2 separate categories, with different treatments for each pathology.
- Nerve sensitisation – normally associated with a traction injury, inflammation of the nerve sheath, or repetitive over-stretching of the nerve. A nerve sensitisation may cause symptoms like burning, shooting, itchy pain.
- Nerve compression (radiculopathy) – caused by a physical structure, such as a disc bulge in the spine, or a tight muscle in the limb, compressing the nerve. A compressed nerve cause symptoms like pins and needles, numbness and weakness.
Disc Bulge
- How does it happen?
A disc can bulge or herniate because of an injury, improper lifting or can occur spontaneously. - Risk Factors
– Age
– Repetitive bending and twisting motions
– Sudden fall or trauma
– Smoking - Common Symptoms
– Pain in the neck, which can radiate down the arm
– Weakness
– Loss of range of motion
– Pins & needles, numbness - Common treatments and recovery expectations
Treatment will depend on the severity of the condition. Acute disc problems; rest, pain management, ice, physical therapy and education. Mild disc issues; rest, ice and pain management may reduce the pain and reduce inflammation along with postural re-education, stretching, strengthening and stabilisation exercises to prevent re-occurrence. - Research
A systematic review conducted in 2014 (Brinjiki et al) found that disc bulges are extremely common in the general population and that there is actually a very poor correlation between pain and the appearance of a disc bulge on MRI. Whilst they can cause pain, they are much more likely to cause referred pain (down the shoulder/arm or leg) than cause spinal pain. If you have been diagnosed with a disc bulge, but are not suffering from any referred pain in the arm or leg, then it is unlikely that the disc is the source of your pain. You would then be classified, according to the diagnostic triage criteria, as having local muscular or joint-related back pain. Disc bulges that do become symptomatic will cause nerve pain and should be treated as a nerve condition (above).
Pelvic and Sacroiliac joint Pain
These conditions generally only affect 2 populations. They are:
- Pregnant or post-partum women.
- Those suffering from ankylosing spondylitis.
It is common for people to complain of their pelvis or hips being “out of place” or “one hip higher than the other”. Much research has been conducted in this area and we are confident now that a) it is almost impossible to tell, without a fine slice CT scan if the pelvis has moved out of place and b) the only scenario where this might occur is during or after pregnancy or after significant physical trauma resulting in hospitalisation. We can now readily identify those who actually are suffering from sacroiliac pain and can be treated effectively with bracing (pre and post-natally) or with stretching and strengthening of the pelvic girdle.